Long-term solutions for building resilience into the drug supply
- Colin Hurd
- 17 March 2026
- 8 Comments
When a life-saving drug disappears from pharmacy shelves, it’s not just an inconvenience-it’s a crisis. In 2022, the U.S. saw 245 drug shortages, and more than half of them involved sterile injectables used in hospitals for emergencies, surgeries, and cancer treatments. These aren’t rare glitches. They’re symptoms of a system built for efficiency, not endurance. The truth is, we’ve spent decades optimizing drug supply chains for low cost and fast delivery, but we never built them to handle shocks. Now, we’re paying for it-with patient lives at risk.
Why the drug supply is so fragile
The modern pharmaceutical supply chain is a global machine, but it’s built on a single, risky premise: make it cheap, make it fast, and trust that nothing will break. About 72% of the active ingredients in U.S. drugs come from outside the country, with nearly 30% of that coming from just two nations-China and India. That means a single flood, political tension, or factory fire halfway across the world can ripple through hospitals here. It’s like building a house on a fault line and calling it safe because the foundation is cheap. The problem isn’t just geography. It’s depth. Only 12% of drug companies know where their raw materials come from beyond three levels deep in the supply chain. That’s like ordering a cake and not knowing if the flour came from a local mill or a warehouse in another country. When disruptions hit, companies can’t see the full picture, so they can’t react fast enough. And when they do react, they often scramble to one supplier, making the whole system even more brittle.What resilience actually looks like
Resilience doesn’t mean building everything in the U.S. or stockpiling every drug. It means designing a system that can bend without breaking. The National Academies of Sciences laid out a clear framework: anticipate, plan, and manage risk. That sounds simple, but it’s not. It requires three concrete actions.- Buffer stockpiles for critical drugs-6 to 12 months’ worth, not just a few weeks. This isn’t hoarding. It’s insurance. For drugs like epinephrine or antibiotics used in emergencies, even a 30-day delay can mean lives lost.
- Supplier diversification-having at least three geographically separate sources for each key ingredient. No single country should control more than 40% of your supply. If one source fails, the others can pick up the slack.
- Manufacturing redundancy-producing the same active pharmaceutical ingredient (API) in two different facilities. For the top 80% of drugs by volume, this isn’t optional anymore. It’s the baseline.
The cost of doing nothing
Some argue that building resilience is too expensive. But the cost of shortages is higher. In 2022, drug shortages cost the U.S. healthcare system an estimated $216 million in extra care, emergency purchases, and delayed treatments. That doesn’t include the human cost-patients waiting for dialysis, cancer patients missing chemo cycles, or newborns in NICUs without life-saving antibiotics. Reshoring all API production would add 25-40% to costs. That’s steep. But you don’t need to bring everything home. A smarter approach is to focus on the most critical drugs. For example, antibiotics, anesthetics, and heart medications-those are the ones that can’t afford delays. The Duke-Margolis Center found that a hybrid model-domestic production for 10-15% of the most vulnerable drugs, paired with diversified international suppliers for the rest-would prevent 85% of shortages at just $1.2-$1.8 billion per year. Compare that to stockpiling everything, which would cost $3.5-$4.2 billion and only stop 45% of shortages.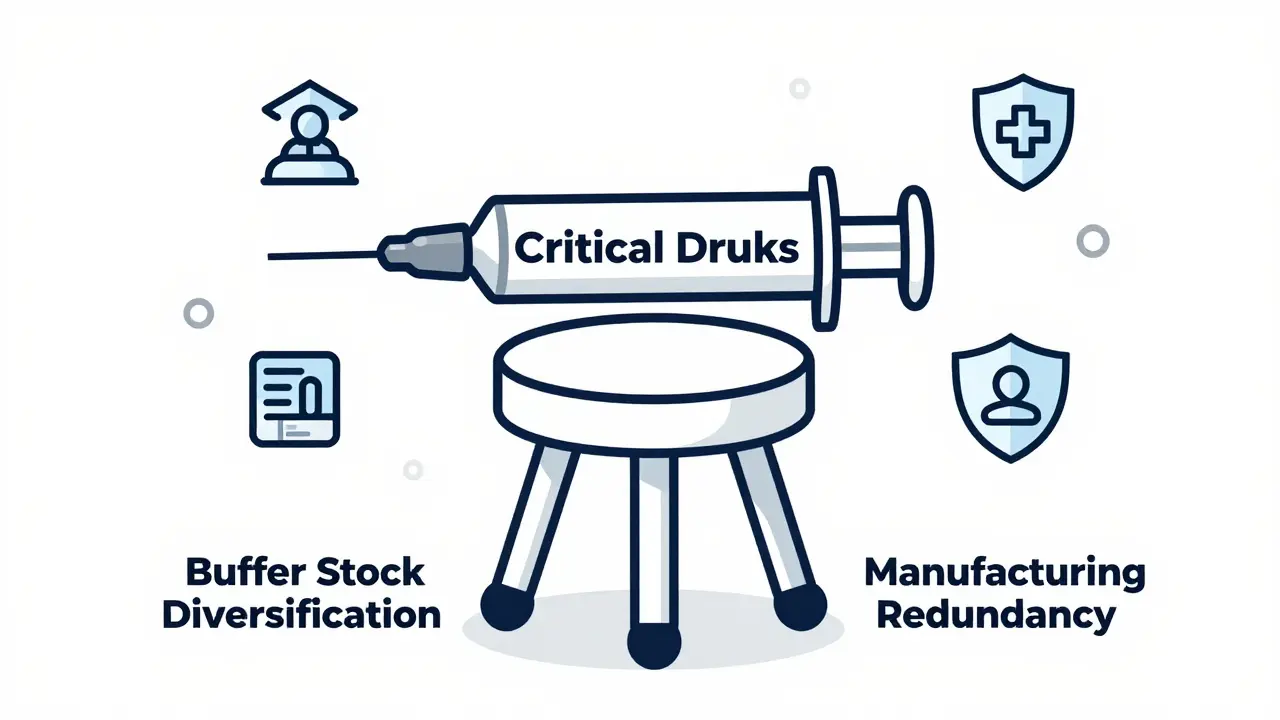
Technology is the hidden key
You can’t manage what you can’t see. Right now, most drug companies only track their direct suppliers (Tier 1). They don’t know who supplies the chemicals to those suppliers (Tier 2), or where the raw materials came from (Tier 3). That’s a massive blind spot. One company that implemented full supply chain mapping saw a 32% drop in disruptions-even though this tech made up only 8% of their resilience budget. AI is making this possible. Predictive models now forecast disruptions with 83% accuracy over 30-day windows. These systems don’t just react-they anticipate. A flood in India? A labor strike in Germany? A cyberattack on a logistics hub? AI can flag these risks before they hit. In 2023, 58% of pharmaceutical companies used AI for supply chain forecasting-up from just 22% in 2021. That’s not a trend. It’s a necessity.Cybersecurity isn’t optional
The supply chain isn’t just vulnerable to natural disasters or political instability. It’s under constant digital attack. Between 2020 and 2023, cyberattacks on healthcare supply chains jumped 214%. Ransomware can lock down a warehouse. Phishing can trick a supplier into redirecting a shipment. A single breach can cut off a drug’s entire pipeline. The solution? Embedding the NIST Cybersecurity Framework into every partner in the chain-not just the big players. The Healthcare Distribution Alliance found that coordinated threat intelligence sharing reduced response times by 47%. That’s not a luxury. It’s a lifeline.Regulations are finally catching up
For years, regulation lagged behind risk. But that’s changing. The FDA’s Drug Supply Chain Security Act (DSCSA) now requires full electronic tracing of every drug package by 2024. That means every bottle, vial, or pill pack will have a digital trail from factory to pharmacy. It’s a massive shift, and it’s forcing transparency. The HHS 2024 Supply Chain Resilience Implementation Plan is allocating $520 million to boost domestic production of 50 critical drugs, aiming for 40% of those APIs to be made in the U.S. by 2027. Meanwhile, CMS is proposing a rule that would tie Medicare reimbursement to supply chain transparency. By 2026, manufacturers will have to disclose where their drugs come from-down to the raw material level. This isn’t bureaucracy. It’s accountability.
What’s working-real examples
Pfizer spent $220 million and 18 months overhauling its supply chain with AI-driven forecasting. Result? A 38% drop in stockouts. Merck used federal incentives to bring domestic production of 12 critical antibiotics back to the U.S. Their cost went up 31%, but they now control 95% of the supply. That’s the trade-off: higher prices now, fewer crises later. Distributors in rural areas started using drones to deliver drugs to pharmacies that used to wait three days for shipments. Emergency delivery times dropped from 72 hours to four. It sounds futuristic, but it’s happening. Regulatory hurdles remain, but the proof is there: innovation works when it’s focused on reliability.The biggest barrier? Money and mindset
The biggest roadblock isn’t technology or policy. It’s incentives. Most hospitals and insurers still buy drugs based on the lowest price per unit. That means manufacturers are punished for investing in resilience-it makes their products more expensive. A hospital might choose a $10 drug from a single-source supplier over a $12 drug with three backup sources. That’s short-term thinking with long-term consequences. Only 35% of companies have staff trained in supply chain risk analytics. And 78% use systems that don’t talk to each other. Without skilled people and connected data, even the best tools fail.The path forward
Building resilience isn’t about one fix. It’s about layers:- Map your supply chain-know where every ingredient comes from.
- Identify your top 20 critical drugs and build redundancy into their production.
- Stockpile 6-12 months of those drugs.
- Use AI to predict disruptions before they happen.
- Secure your digital systems like you secure your physical warehouses.
- Push for payment models that reward reliability, not just low cost.
Why do drug shortages keep happening?
Drug shortages happen because the supply chain is built for efficiency, not resilience. Most drugs rely on a single supplier for their active ingredient, often located overseas. When a factory shuts down, a shipment gets delayed, or a natural disaster hits, there’s no backup. With 72% of active pharmaceutical ingredients (APIs) made outside the U.S., and only 12% of companies tracking beyond their first-tier suppliers, the system has no safety net. It’s not random-it’s structural.
Is reshoring drug manufacturing the best solution?
Not for everything. Bringing all API production back to the U.S. would raise costs by 25-40%, which isn’t sustainable. The smarter approach is to reshore only the most critical drugs-like antibiotics, anesthetics, and emergency medications. For the rest, diversify suppliers across multiple countries. A hybrid model-domestic production for high-risk drugs plus international diversification for others-prevents 85% of shortages at a fraction of the cost of full reshoring.
How much of a buffer stock do we really need?
For critical drugs-especially sterile injectables used in hospitals-a 6- to 12-month stockpile is the recommended minimum. This isn’t about hoarding; it’s about covering disruptions that take weeks or months to resolve. Stockpiling everything is too expensive and inefficient. But targeting just the top 20% of drugs by clinical impact can prevent over 70% of shortages. The goal is to have enough to bridge the gap until production resumes.
Can AI really prevent drug shortages?
Yes, if it’s used correctly. AI models now predict supply chain disruptions with 83% accuracy over 30-day windows. They analyze weather patterns, geopolitical events, shipping delays, and even social media trends to flag risks before they escalate. Companies using AI for forecasting report 32% fewer disruptions. It’s not magic-it’s data. The key is integrating AI with real-time supply chain mapping, not using it in isolation.
Why isn’t everyone doing this already?
Two main reasons: cost and incentives. Building resilience costs money-up to $1.8 billion a year for the full system. But most buyers still choose the cheapest drug, not the most reliable one. Manufacturers get punished for investing in redundancy. Also, 78% of companies use incompatible data systems, and only 35% have staff trained in risk analytics. Without aligned incentives and better tools, change is slow.
What role do governments play in fixing this?
Governments are shifting from bystanders to catalysts. The U.S. HHS is investing $520 million to boost domestic production of 50 critical drugs. The FDA now requires annual vulnerability assessments from manufacturers. CMS is moving to tie Medicare payments to supply chain transparency-forcing companies to disclose where their drugs come from. These aren’t just regulations. They’re market signals: resilience is now a requirement, not a bonus.


Comments
Kal Lambert
Buffer stockpiles for critical drugs? Absolutely. 6-12 months isn't excessive-it's basic insurance. We do it for fuel, for food, for ammo. Why not for epinephrine or antibiotics?
Stop treating healthcare like a stock market. Lives aren't shares.
March 19, 2026 AT 03:17
Melissa Stansbury
I work in a rural ER and let me tell you-we’ve had to reroute cardiac arrest patients because we ran out of norepinephrine. It’s not theoretical. It’s 3am and your patient’s BP is crashing and the pharmacy says ‘back in 14 days.’
Resilience isn’t a buzzword. It’s the difference between life and a funeral notice.
March 19, 2026 AT 06:28
cara s
It is, indeed, a profoundly concerning and deeply systemic issue that has been exacerbated by decades of neoliberal economic policy prioritizing shareholder value over public health infrastructure.
One must consider that the global pharmaceutical supply chain, as currently constituted, is not merely inefficient-it is structurally vulnerable due to its hyper-optimization for cost-reduction at the expense of redundancy, transparency, and resilience.
Moreover, the fact that only twelve percent of manufacturers can trace their supply chains beyond the third tier is not an oversight-it is a deliberate choice made to obscure liability and avoid accountability.
AI forecasting, while promising, is not a panacea; it is merely a bandage on a hemorrhaging artery unless paired with regulatory enforcement and capital investment.
The HHS allocation of five hundred twenty million dollars is commendable, yet it pales in comparison to the $216 million in ancillary costs incurred annually due to shortages.
Furthermore, the FDA’s DSCSA mandate, while a step forward, is woefully underfunded and lacks teeth in terms of penalties for noncompliance.
It is my firm conviction that without mandatory public disclosure of Tier 3 sourcing and enforced multi-sourcing requirements, we are merely rearranging deck chairs on the Titanic.
And yet-I remain cautiously optimistic, because change, however slow, is now being recognized as inevitable.
Human lives are not commodities. And if we continue to treat them as such, we deserve the consequences.
Let us not forget: the first casualty of war is truth. The first casualty of profit-driven healthcare is trust.
And we are losing both.
March 19, 2026 AT 21:16
Amadi Kenneth
Let’s be real-this whole drug shortage thing? It’s not an accident. It’s a plan.
Big Pharma and the government? They’re letting shortages happen so they can push you into expensive alternatives.
China? India? They’re just pawns. The real players are in Wall Street boardrooms.
And don’t you dare think the FDA’s new tracing rules are about transparency-they’re about tracking YOU, not the supply chain.
AI? That’s surveillance with a lab coat.
They want you dependent. They want you scared. They want you to pay more.
And if you’re not angry about this… you’re not paying attention.
They’re not fixing the system.
They’re monetizing the collapse.
March 21, 2026 AT 19:09
Shameer Ahammad
It is a matter of grave concern that the United States continues to rely on foreign sources for 72% of its active pharmaceutical ingredients, particularly when the geopolitical instability of China and India is well-documented.
Furthermore, the notion that ‘diversification’ is sufficient is fundamentally flawed-supply chains are not portfolios, and risk cannot be mitigated through statistical averaging.
One must consider that India, despite its pharmaceutical prowess, suffers from chronic infrastructure deficiencies-including power outages, labor strikes, and environmental degradation-all of which directly impact manufacturing consistency.
Moreover, the claim that AI forecasting is ‘83% accurate’ is misleading-it does not account for black swan events, such as cyberattacks or sudden regulatory bans.
The only ethical, sustainable, and scientifically sound solution is full domestic production of all critical APIs-no exceptions.
Reshoring is not ‘expensive’-it is an act of national sovereignty.
And anyone who argues otherwise is either complicit or dangerously naive.
March 23, 2026 AT 17:26
Manish Singh
As someone from India who works in pharma, I see both sides.
Yes, we make a lot of APIs-but we’re not the problem. We’re the backbone.
Our factories follow WHO-GMP. Our workers are skilled. But we get blamed because it’s easier than fixing the U.S. system.
Instead of calling us risky, why not invest in joint quality audits? Build mutual trust?
And yes-we need redundancy. But not because we’re untrustworthy. Because no single country should hold that much power.
Let’s stop the us-vs-them nonsense. This isn’t a war. It’s a supply chain.
And we all need to fix it-together.
March 24, 2026 AT 05:21
Nilesh Khedekar
ai is a scam… they say it predicts disruptions but what they really mean is they use it to predict when youll run out so they can jack up prices…
and dont get me started on the fda… they’re just there to make sure big pharma stays in charge…
they dont care if you die… they care if the stock goes up…
theyll let you wait 30 days for antibiotics… then sell you the same drug for 5x the price…
its all a game… and we’re the pawns…
and now they want us to pay more for ‘resilience’… yeah right…
they’re not fixing the system… they’re just making it more expensive to fix
March 25, 2026 AT 05:50
Robin Hall
It is my professional assessment that the current regulatory framework is fundamentally inadequate to address the systemic vulnerabilities inherent in the global pharmaceutical supply chain.
The FDA’s Drug Supply Chain Security Act, while a step in the correct direction, remains non-binding in its enforcement mechanisms and lacks mandatory third-party verification protocols.
Furthermore, the allocation of $520 million by HHS for domestic production is insufficient to achieve the stated goal of 40% domestic API production by 2027, given that capital expenditures for FDA-compliant manufacturing facilities average $450 million per site.
Moreover, the integration of AI into supply chain forecasting-while technologically sophisticated-remains susceptible to data poisoning and algorithmic bias, particularly when training data is sourced from proprietary, non-transparent vendor systems.
Therefore, I must conclude that without the establishment of a federally mandated, auditable, real-time supply chain transparency registry-with penalties for non-compliance-the entire initiative is an exercise in performative governance.
And if we are to preserve public health integrity, we must demand more than optimism.
We must demand accountability.
March 25, 2026 AT 19:32