Retinal Vein Occlusion: Understanding Risks and Injection Treatments

- Colin Hurd
- 1 April 2026
- 14 Comments
The Silent Threat to Your Vision
Suddenly losing sight in one eye can feel like the world went dark without warning. You might wake up, blink, and realize half your view is blurry or gone completely. This frightening experience often points to a blockage deep inside the eye known as Retinal Vein OcclusionA condition where veins draining blood from the retina get blocked. Also known as RVO, this vascular disorder affects roughly 16 million people worldwide. Unlike a cataract that creeps in slowly, RVO hits hard and fast. It is essentially a stroke affecting the tiny blood vessels at the back of your eye.
What Exactly Is Happening?
To understand the damage, imagine the RetinaThe light-sensitive tissue layer at the back of the eye as a garden hose system. Water flows in, does its job, and flows out. In RVO, the drainage pipes get clogged. When blood cannot exit the retina efficiently, it backs up. This pressure causes fluid to leak into sensitive areas, leading to swelling called macular edema. This swelling distorts your vision and, if left unchecked, causes permanent damage.
There are two main ways this blockage happens. In Central Retinal Vein OcclusionBlockage of the main vein draining the retina, or CRVO, the primary drain is obstructed. This is serious and affects the whole eye. In Branch Retinal Vein OcclusionBlockage of smaller branch veins in the retina, or BRVO, a smaller pipe gets pinched off. While less extensive than CRVO, BRVO still impacts the central vision area significantly. Over 90% of CRVO cases happen in patients over 55 years old, making age the biggest predictor of risk.
Why Does It Happen to You?
You might wonder if you did anything wrong. Often, RVO is the result of long-term wear and tear on your blood vessels rather than a single mistake. High blood pressure is the number one culprit. Statistics show that up to 73% of older patients diagnosed with RVO also struggle with uncontrolled hypertension. Think of high pressure as hammering your vessel walls until they weaken and become prone to clotting.
Beyond blood pressure, several other factors stack the deck against you. Diabetes MellitusA chronic condition affecting blood sugar levels is present in about 10% of RVO patients over 50. High cholesterol, defined medically as total cholesterol over 6.5 mmol/l, appears in 35% of cases regardless of age. Even smoking contributes, with reports linking 25-30% of RVO cases to tobacco use. These aren't just separate checkboxes; they work together.
If you are younger, say under 45, the story changes slightly. About 5-10% of RVO cases occur in this group, often linked to different causes. For women in this demographic, oral contraceptive use is a significant association with central vein occlusion. Additionally, blood clotting disorders like polycythemia vera or factor V Leiden deficiency play a much larger role when age isn't the primary driver. Understanding these links helps you know which tests matter most during a diagnosis.
| Risk Factor | Relevance in Older Adults (Over 50) | Relevance in Younger Adults (Under 45) |
|---|---|---|
| Hypertension | Present in 73% of cases | Present in 25% of cases |
| Diabetes | Affects 10% of patients | Uncommon occurrence |
| Blood Disorders | Rare cause | Increasing relevance |
The Gold Standard: Eye Injections
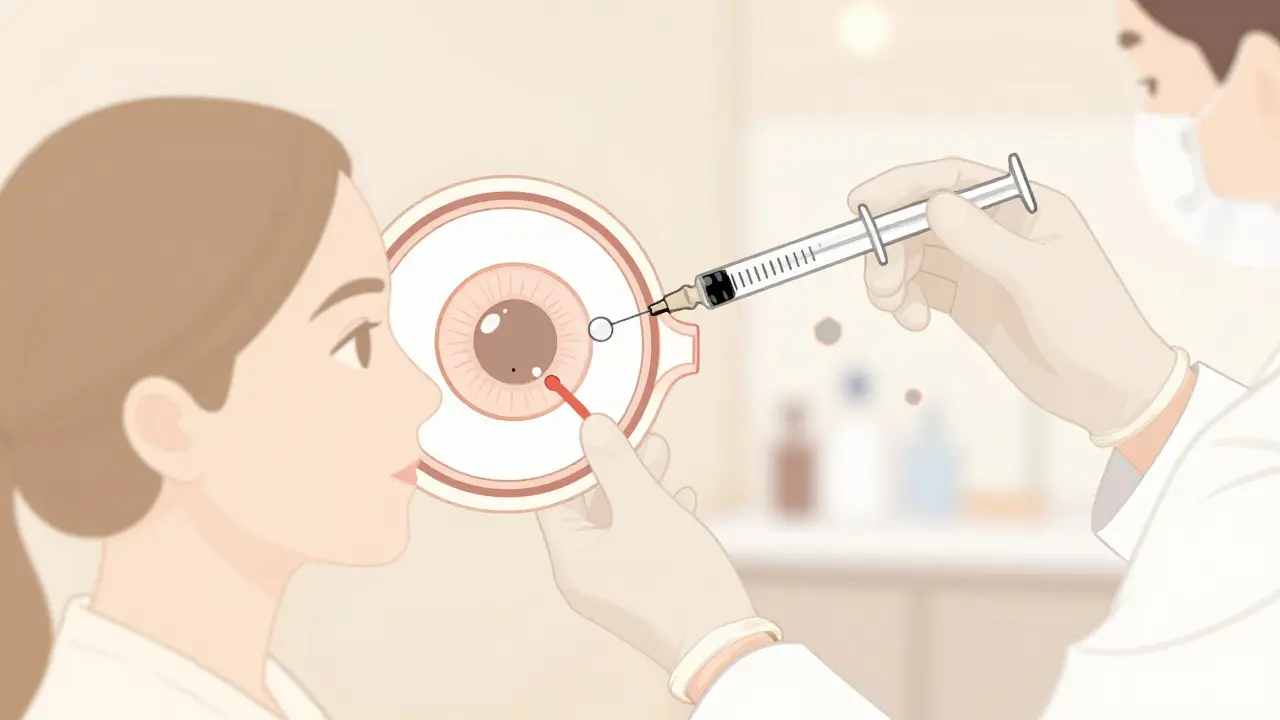
Once the doctor confirms the diagnosis using an optical coherence tomography (OCT) scan, action is required. The goal isn't always to unblock the vein itself, but to stop the leakage caused by the blockage. This is where Anti-VEGF TherapyMedication that blocks vascular endothelial growth factor comes in. These drugs stop the chemical signals that tell blood vessels to grow weak and leaky.
You will likely hear three names mentioned frequently. RanibizumabA branded medication also known as Lucentis (Lucentis) was a pioneer in this space, approved specifically for RVO back in 2010. AfliberceptA medication marketed as Eylea for eye conditions (Eylea) followed, with trials like GALILEO showing patients could gain an average of 16 letters on vision charts compared to sham treatment. Then there is BevacizumabOff-label cancer drug used widely in retinal care (Avastin), which costs significantly less per dose but is technically an off-label use for eyes in many regions.
The procedure involves injecting this medicine directly into the eye. Sounds scary, right? Most offices are incredibly routine about this. They prep your eye with numbing drops and a sterile antiseptic solution. The actual needle stays in for just seconds. Despite the brief duration, anxiety is common. Surveys show about 41% of patients report treatment fatigue after a year. However, the results speak volumes: 78% of RVO patients reported significant vision improvement after 12 months of anti-VEGF therapy according to registry data.
Alternative Paths: Steroids and Implants
Sometimes injections alone don't clear the waterlogged retina. In these stubborn cases, doctors turn to corticosteroids. A popular option is the dexamethasone implant, commonly known by the brand name OzurdexA steroid implant delivered into the eye. Unlike liquid injections that wear off quickly, this implant slowly releases medication over several months. Studies like the GENEVA study showed nearly 28% of CRVO patients gained 15 lines of vision using this method compared to just 13% with a placebo.
However, steroids come with their own set of trade-offs. Because they suppress inflammation differently than anti-VEGF agents, they carry a higher risk of raising intraocular pressure (glaucoma) or accelerating cataract formation. Long-term monitoring is non-negotiable. Your doctor might choose this route if you have poor response to monthly shots or if you have a history of severe dry eye that worsens with frequent needling.
Navigating Costs and Commitment
Treating RVO is rarely a one-time fix. Real-world data suggests patients need between 8 to 12 injections annually for optimal outcomes. This frequency creates a financial reality check. The cost gap between drugs is stark. Generic bevacizumab might cost around $50 per dose, whereas brand-name ranibizumab or aflibercept can hit $2,000 per shot in some markets. This price difference drives choice in safety-net hospitals versus private clinics.
Patient forums reveal a mixed bag of feelings regarding the burden. Some users share stories of improved vision from 20/200 to 20/60, calling it life-saving despite the cost. Others describe missing appointments due to "injection anxiety." It is a marathon, not a sprint. New technologies aim to change this frequency. Devices like the Port Delivery System (Susvimo) are in trials, promising to stretch dosing from every month to every quarter. Gene therapy trials are also exploring sustained release methods to eliminate visits altogether.
Summary
Retinal Vein Occlusion is a serious vascular event that demands immediate attention. By understanding your risk profile-managing blood pressure, controlling diabetes, and avoiding smoking-you mitigate chances of onset. When blockage occurs, modern medicine offers robust tools. Whether through anti-VEGF agents or steroid implants, restoring vision is often possible if treated early. Stay proactive with your eye exams, especially as you enter your mid-50s.
Is Retinal Vein Occlusion reversible?
While the actual vein blockage may not reopen spontaneously, the resulting vision loss can often be reversed. Timely treatment of the macular edema (swelling) allows vision to recover. Delay increases the chance of permanent nerve damage.
How many injections do I need?
Most protocols suggest starting with monthly injections until swelling resolves. After stabilization, many move to an as-needed basis. On average, patients receive 8 to 12 injections per year.
Are eye injections painful?
Doctors use numbing drops before the procedure. Patients often report feeling mild pressure rather than sharp pain. Anxiety is usually worse than the physical sensation of the needle.
Can RVO affect both eyes?
RVO usually occurs in one eye initially. However, having risk factors puts the second eye at risk. Roughly 10% to 20% of patients develop RVO in the fellow eye over time.
What symptoms should trigger a doctor visit?
Seek help immediately for sudden painless vision loss, blurriness, or distortion. RVO symptoms appear quickly and require urgent intervention to save sight.




Comments
Mark Zhang
I know how scary sudden vision changes can feel for anyone experiencing this. Seeing the world blur out like that is genuinely terrifying without warning signs beforehand. My cousin went through something similar and found immediate treatment made all the difference. Getting checked out quickly prevents permanent damage from taking hold too strongly. It is important to trust the medical team when they suggest the injection therapy options available. Most people report feeling relief once the swelling finally starts to subside. You never have to walk this path alone if you reach out for community support.
April 2, 2026 AT 21:34
simran kaur
These pharmaceutical companies push these expensive injections just to maximize their profit margins annually. They know the average patient cannot afford the brand name versions easily. There is a pattern here where they prioritize revenue over actual long term health outcomes for us. Anti VEGF drugs seem to create dependency rather than curing the underlying blockage issues completely. People should research alternative methods before signing up for monthly visits blindly.
April 3, 2026 AT 15:54
Jenna Carpenter
you dont knw wat u r talkin about teh doctors r right
April 4, 2026 AT 04:53
Ace Kalagui
I heard my uncle had this condition last year and it changed everything for him. He woke up one morning unable to see the clock on the wall without squinting hard. The doctor told him immediately that it was likely a vein occlusion issue. They ran a bunch of tests right away to confirm the diagnosis before doing anything else. He was really scared about the needles they were going to put in his eye. I remember him saying he felt like he was in trouble more than usual. But the results were surprisingly positive after the first few treatments started working well. The swelling went down significantly within a couple of weeks according to his reports. He did have to come in quite often though for the monthly shots initially. It got to be a bit of a hassle to schedule appointments around work hours. Eventually the dosage frequency dropped off once the fluid stabilized completely. He still worries about the pressure spikes but feels much better now overall. Cost was definitely a major factor since insurance barely covered half the price. We managed to find a cheaper clinic nearby that used generic alternatives for the injections. Now he reads daily without needing thick glasses for near vision again. You have to stay consistent because stopping early means losing progress fast.
April 4, 2026 AT 17:46
Sam Hayes
lots of people forget to mention the numbing drops help a ton during the procedure itself. the sterility of the room matters more than worrying about pain really. just try to relax while the nurse prepares the site for entry. i have seen many patients panic unnecessarily before the needle goes in. anxiety is often worse than the actual physical sensation of the shot
April 5, 2026 AT 19:37
Vicki Marinker
The statistics regarding glaucoma risk are alarmingly high for implant patients specifically. Corticosteroids offer temporary relief but carry significant long term structural damage risks. Many individuals overlook the cataract acceleration rate associated with repeated steroid use. It is a calculated gamble that favors short term gains over eye health preservation. The burden of monitoring intraocular pressure shifts entirely onto the patient eventually.
April 7, 2026 AT 05:49
Aysha Hind
It is clear that mainstream medicine wants to keep patients on a cycle of costly treatments indefinitely. The implant strategy locks people into frequent monitoring visits that benefit the clinics financially. There is a deeper motive behind prioritizing these invasive solutions over less aggressive interventions. Why would they recommend anything that does not require a return visit every month? We are essentially funding a permanent revenue stream with our own vision health.
April 7, 2026 AT 11:58
Lawrence Rimmer
Aging brings unavoidable decay to our delicate internal systems including the vascular network. We must accept that fragility is part of the human condition as years accumulate. Fighting the natural course of biological decline often leads to greater frustration than acceptance would. The search for a cure is noble but prevention is the wiser philosophical approach ultimately.
April 9, 2026 AT 05:43
Hudson Nascimento Santos
While the physical symptoms dominate the conversation, the psychological toll is often ignored by clinicians. Mental resilience becomes just as critical as physical compliance with medication schedules. We exist in a state of flux where control is an illusion anyway. Understanding this duality might ease some of the burden placed on families caring for affected relatives.
April 10, 2026 AT 12:47
Brian Shiroma
Of course the insurance providers love charging premium rates for the brand name drugs exclusively. They know generics cost fifty dollars but push the two thousand dollar option instead. It is hilarious how they call it standard care while bleeding patients dry financially. Nobody seems to ask why the price gap exists beyond vague patent explanations. The system is designed to extract every penny possible from vulnerable populations.
April 10, 2026 AT 23:21
Rachelle Z
Totally agree with that point about the money stuff! 😩💸 It is such a nightmare dealing with insurance co-op. 👎🙄 Everyone complains about prices here online. 🙃 Hope you get better results soon!!! ✨💕
April 11, 2026 AT 08:45
Branden Prunica
I lost almost everything I could see on my left side in a matter of minutes one Tuesday morning. The silence of the darkness was louder than any scream I could have imagined making. Walking through my house became an exercise in absolute terror and vulnerability immediately. I cried so much that my face swelled up for days afterwards from the sheer stress. Doctors said it would get better but watching your sight leave you is devastating.
April 11, 2026 AT 19:59
Beth LeCours
That sounds like a terrible thing to go through honestly.
April 12, 2026 AT 18:59
angel sharma
Staying motivated during this journey is absolutely crucial for recovery success rates too. Many people give up before they even reach the maximum potential visual acuity levels possible. It requires patience and discipline that most folks simply do not possess nowadays. You must trust the process even when you feel like nothing is changing inside your eye. The medicine works slowly over time to reduce the harmful leaks effectively. Do not listen to skeptics who claim the injections are harmful nonsense procedures. Your retina is fragile tissue that needs protection from damaging swelling constantly. Every visit adds another layer of safety against permanent damage occurring later on. Keep track of your blood pressure numbers daily at home without fail always. Stress management plays a huge role in keeping your vascular system healthy overall. Meditation helps calm the mind while you wait for appointment times to arrive soon. Eat foods rich in antioxidants that support retinal health naturally without extra cost. Drink plenty of water to maintain blood flow consistency throughout your entire body system. Sleep well at night so your eyes can rest fully during dark hours daily. Stay connected with others facing similar challenges for emotional support throughout the whole experience. Together we can navigate these medical hurdles with strength and hope for tomorrow ahead.
April 13, 2026 AT 00:47