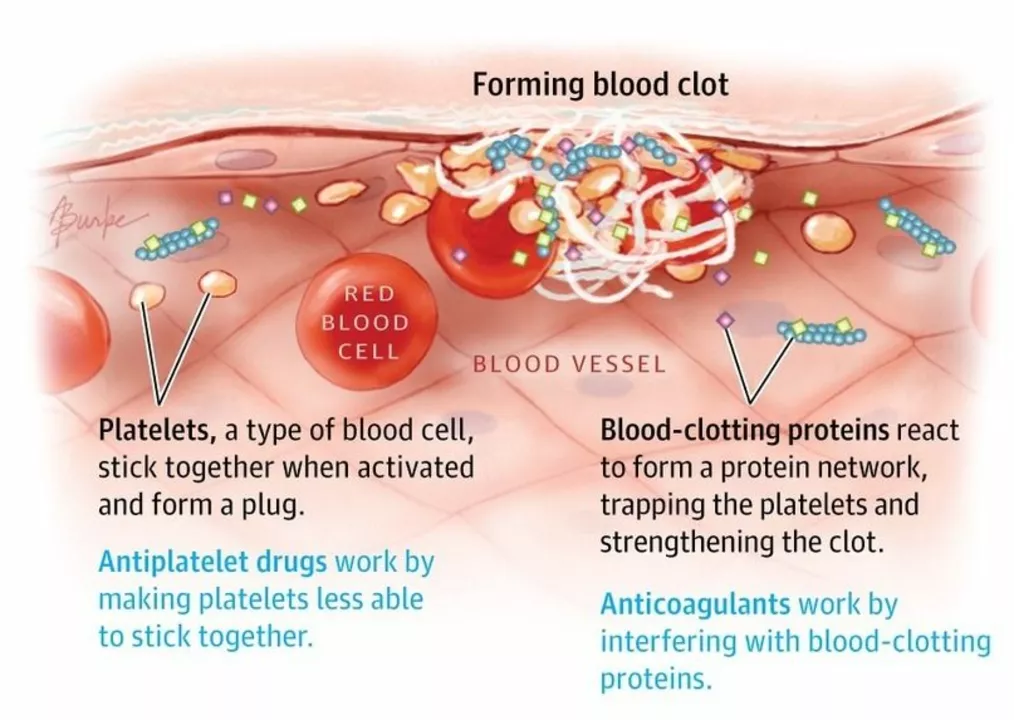
Blood Clot Formation: What Causes Clots and How to Spot Them
Blood clots are your body’s emergency response when a blood vessel gets injured — useful in small doses, dangerous when they form inside vessels without an injury. Clots in veins (venous clots) behave differently from clots in arteries. Venous clots often start in the legs and can travel to the lungs. Arterial clots can block blood to the heart or brain and cause a heart attack or stroke. Knowing the difference helps you act fast.
What causes clots and who’s at risk?
Clots form when three things line up: slow blood flow, vessel wall damage, and blood that’s more likely to clot. Common risks include long bed rest or long flights, recent surgery, cancer, pregnancy, using estrogen-based birth control, smoking, obesity, and certain genetic conditions called thrombophilias. Older age raises risk too. If you have any of these, tell your doctor — prevention is often simple and effective.
Medications can change your clot risk. Antiplatelet drugs (like prasugrel) mainly prevent arterial clots after stents or heart attacks. Anticoagulants (blood thinners) target venous clots and are the main treatment for deep vein thrombosis (DVT) and pulmonary embolism (PE). Never stop or start these meds without talking to your provider.
How clots are found and treated
Symptoms depend on where the clot is. A DVT in the leg typically causes swelling, warmth, redness, and pain or heaviness. A pulmonary embolism often shows as sudden shortness of breath, sharp chest pain that gets worse when you breathe, a fast heartbeat, lightheadedness, or coughing up blood. These need urgent care.
Doctors use tests to confirm a clot. A D-dimer blood test helps rule out clots when the chance is low. Ultrasound (venous duplex) is the usual test for leg clots. For suspected lung clots, CT pulmonary angiography is the go-to scan. Treatment depends on severity: most people start anticoagulants such as heparin, low-molecular-weight heparin, warfarin, or newer direct oral anticoagulants like apixaban or rivaroxaban. In massive pulmonary embolism, clot-busting drugs or procedures may be needed. An IVC filter is sometimes used when blood thinners aren’t an option.
Preventing clots is often about small habits. Move your legs on long trips, get up and walk after surgery when your team says it’s safe, wear compression stockings when advised, stay hydrated, quit smoking, and manage weight. If you’re on hormone therapy or have a family history of clots, ask your doctor about safer options or extra monitoring.
If you’re worried about clot risk or notice warning signs, get medical help. Quick diagnosis and the right treatment cut the risk of serious complications. Want more on meds like prasugrel or how blood thinners work? Check our detailed guides for plain-language answers and practical tips.
- Colin Hurd
- May, 16 2023
- 8 Comments
The connection between smoking and blood clot formation
As a blogger, I've recently been researching the connection between smoking and blood clot formation. It turns out that smoking can significantly increase the risk of blood clots by damaging the lining of blood vessels and causing them to narrow. Additionally, smoking also increases the levels of fibrinogen, a protein that contributes to clot formation. This, combined with reduced blood flow due to nicotine, makes it easier for clots to form and block blood vessels. It's clear that quitting smoking is essential for lowering the risk of blood clot formation and maintaining overall health.