Menstrual cycle — what to expect and how to manage it
Most people hear "28 days" and assume that’s the rule. Reality: a typical cycle is about 24–38 days. Your period is one clear sign your body is cycling, but how it happens, what’s normal, and when to worry are worth knowing.
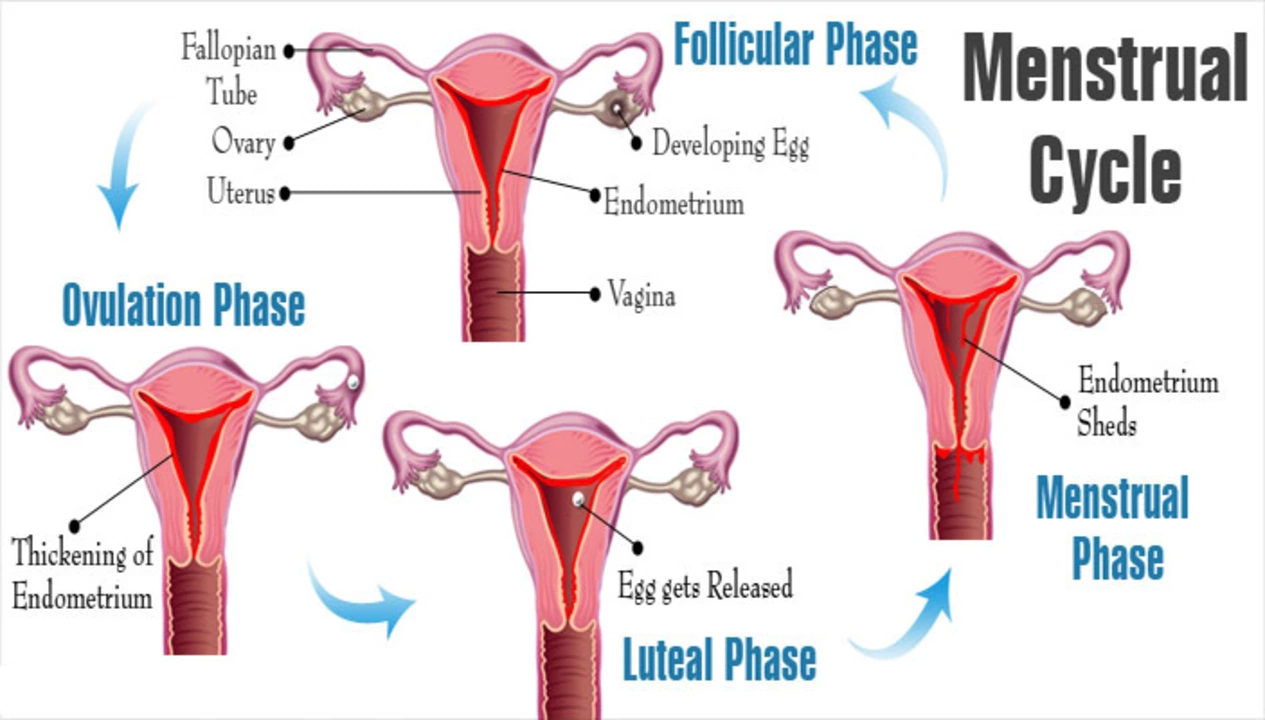
The cycle has four simple parts: the follicular phase (the body prepares an egg), ovulation (the egg is released), the luteal phase (hormones rise to support pregnancy), and menstruation (the lining sheds). Hormones—mainly estrogen and progesterone—drive those steps. Timing can shift from month to month, especially in teens, new moms, or during stress.
Common problems and when to get help
Irregular periods: occasional changes are normal. See a doctor if cycles are consistently shorter than 21 days, longer than 38 days, or stop entirely for months without pregnancy. Missing a period can mean pregnancy, hormonal imbalance, heavy exercise, or certain medicines.
Heavy bleeding: replaceing a pad or tampon every hour for several hours, passing large clots, or bleeding that lasts much longer than usual is too much. That can cause low iron or need medical care.
Severe pain: cramping that stops you from working or sleeping isn’t just "bad cramps." Get checked for conditions like endometriosis or fibroids if pain is persistent or worsening.
Spotting between periods, very light cycles, or new changes after starting a birth control method are worth discussing with your clinician too. Also mention if you have fever, fainting, or very heavy dizziness—those are red flags.
Practical tips: tracking, pain relief, and medicine effects
Track your cycle for three months. Use a calendar, a simple app, or a symptom journal noting flow, pain level, mood, and medications. Tracking helps spot patterns and gives clear info for your doctor.
For cramps and pain, try over-the-counter NSAIDs like ibuprofen, using them at the first sign of cramping. Heat packs, light exercise, and steady sleep help too. If OTC options don’t work, discuss prescription treatments with your clinician.
Birth control changes periods: combined pills, patches, and rings often make periods lighter or more regular. IUDs can reduce bleeding or sometimes cause irregular spotting at first. Some non-hormonal drugs and a few medical conditions also change cycles—tell your provider about all medicines you take.
When you see a clinician, bring your tracking notes: cycle length, flow, pain scale, and any meds. That saves time and gets you to the right tests faster. If you’re worried now—bleeding heavily, fainting, or pregnant with unusual pain—seek care sooner rather than later.
Understanding your cycle gives you more control. Track, try simple fixes for pain, and get help when patterns change. Your period can tell you a lot—listen to it.
- Colin Hurd
- May, 13 2023
- 16 Comments
The Impact of Levothyroxine on Menstrual Cycle: What Women Should Know
As a woman, I recently came across the connection between Levothyroxine and its impact on our menstrual cycle. Levothyroxine is a medication commonly prescribed for thyroid issues, which can significantly affect our periods. In some cases, it can lead to heavier or more irregular cycles, while in others, it might help regulate them by addressing the underlying thyroid issue. It's important for us to understand how our bodies react to this medication and to communicate with our healthcare providers about any changes we experience. By doing so, we can better manage our thyroid health and its effects on our menstrual cycle.