Why Hospital Pharmacies Face the Worst Injectable Medication Shortages
- Colin Hurd
- 15 April 2026
- 0 Comments
Imagine a surgeon scrubbing in for a critical procedure, only to be told the anesthetic is missing. Or a chemotherapy patient arriving for a life-saving infusion, but the clinic has to postpone the session because the drug simply isn't there. This isn't a hypothetical scenario; it's a daily reality for thousands of healthcare providers. While most of us only think about drug shortages when a retail pharmacy says a prescription will be ready "next week," the crisis inside hospital walls is far more severe. Injectable medication shortages aren't just an inconvenience-they are a systemic failure that puts the most vulnerable patients at risk.
The disproportionate burden on hospitals
Why are hospitals suffering more than your local drugstore? It comes down to the type of medicine they use. Retail pharmacies mostly deal with pills and liquids, but hospitals rely heavily on Sterile Injectables is medications administered via injection or infusion that must be completely free of microorganisms and pyrogens. These products make up about 60% of all drugs currently in shortage. Because these meds are injected directly into the bloodstream or muscle, there is zero room for error in quality or sterility.
The numbers are staggering. While a community pharmacy might see 15-20% of its inventory affected by supply issues, hospital pharmacies are reporting that 35-40% of their essential medications are hard to find. For Academic Medical Centers, the impact is even worse. Because they handle the most complex cases, they need a wider variety of specialized injectables, making them 2.3 times more likely to feel a severe clinical impact compared to smaller community hospitals.
Why sterile injectables vanish from shelves
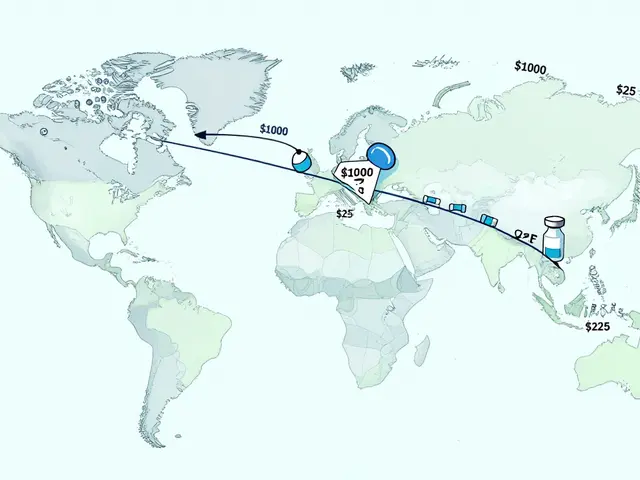
You might wonder why a basic solution like saline or a critical chemotherapy drug would suddenly disappear. It isn't usually one single reason, but a combination of technical and economic failures. The US Pharmacopeia (USP) identifies a few primary culprits: low pricing, manufacturing complexity, and geographic concentration.
First, the profit margins for generic sterile injectables are razor-thin-often just 3-5%. When a manufacturer makes almost nothing on a product, they have no incentive to invest in better equipment or backup facilities. Second, making these drugs is incredibly hard. It requires aseptic processing in highly controlled environments. One small mistake in a cleanroom can lead to a total shutdown of production for months.
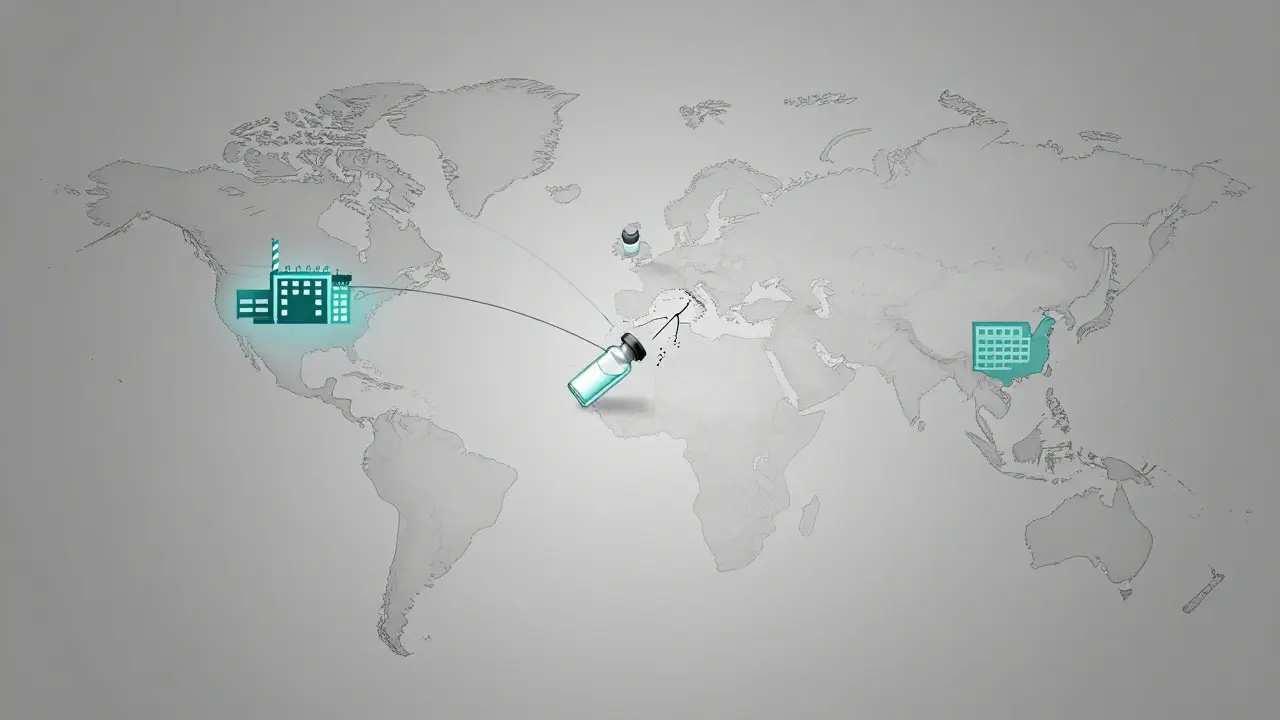
Then there is the "single point of failure" problem. About 80% of active pharmaceutical ingredients for generics come from China and India. If a factory there shuts down due to quality issues, the rest of the world feels it immediately. We've seen this play out in real-time: a tornado hitting a Pfizer plant in North Carolina wiped out 15 critical medications, and quality failures at a facility in India led to a nationwide lack of cisplatin, a vital cancer drug.
| Metric | Retail/Community Pharmacy | Hospital Pharmacy |
|---|---|---|
| Inventory Affected | 15-20% | 35-40% |
| Primary Product Type | Oral/Topical | Sterile Injectables |
| Treatment Impact | Delayed refill/Switch | Postponed surgery/Critical delay |
| Substitution Ease | Relatively High | Low (requires committee approval) |
The hidden cost: Burnout and ethical dilemmas
The crisis doesn't just affect patients; it's breaking the people providing the care. Hospital pharmacists are spending an average of nearly 12 hours a week just chasing down alternative suppliers and managing substitutions. That's a full day and a half of work every week spent on logistics instead of patient care.
More disturbingly, these shortages create a moral burden. About 68% of hospital pharmacists report facing ethical dilemmas over how to allocate a dwindling supply of a drug. In some cases, 42% have had to use less effective alternatives, knowing it might compromise the patient's outcome. Imagine the stress of deciding which patient gets the last vial of a critical medication. This level of pressure leads to rapid burnout and a workforce that feels unsupported by the larger healthcare system.

How hospitals are fighting back
Since they can't wait for the government to fix the supply chain, hospitals have had to get creative. Many have formed formal shortage management committees to decide on "therapeutic interchanges"-which is basically a fancy way of saying they've pre-approved a backup drug if the primary one isn't available.
Some common strategies include:
- Consolidating stock: Keeping scarce items in one secure location rather than spreading them across various wards.
- Tiered allocation: Prioritizing the most critically ill patients for the remaining stock.
- Alternative sourcing: Building direct relationships with smaller or international suppliers to bypass the usual wholesalers.
These steps help, but they aren't a cure. Implementing these protocols takes months of effort and only reduces clinical disruption by about 15-20%. For many, it's like trying to plug a leaking dam with a few pieces of tape.
The road ahead: Will it get better?
There is some hope, but it's cautious. The FDA is attempting to implement a Strategic Plan for Drug Shortage Prevention, and the U.S. government has allocated $1.2 billion to boost domestic manufacturing. The goal is to stop relying so heavily on overseas factories.
However, building a sterile manufacturing plant isn't like opening a coffee shop; it takes years. Analysts suggest it will be 3 to 5 years before these investments actually put more drugs on the shelves. Meanwhile, geopolitical tensions and extreme weather events continue to threaten the few factories that remain. Until the industry moves away from the "lowest price at all costs" model, hospital pharmacies will likely remain the hardest hit part of the system.
Why can't hospitals just substitute one injectable drug for another?
Unlike tablets, where a pharmacist can often switch a brand or a similar generic easily, injectables have different bioavailability and stability profiles. Substituting an IV medication often requires a formal review by a Pharmacy and Therapeutics (P&T) committee to ensure the alternative is safe and effective for the specific patient population.
Which types of medications are most commonly affected?
The hardest-hit categories are anesthetics (with an 87% shortage rate), chemotherapeutic agents (76%), and cardiovascular injectables (68%). These are all critical for acute hospital care and surgery.
How does the geographic location of factories contribute to shortages?
About 80% of active pharmaceutical ingredients (APIs) for generic drugs are manufactured in China and India. This creates a massive vulnerability; if a single region faces a natural disaster, a political shift, or a quality-control shutdown, there are no domestic alternatives to pick up the slack.
What is the "batteries-included" approach to shortage management?
While not a formal term, it refers to the comprehensive strategies hospitals use, such as creating tiered allocation systems, revising standing order sets to include alternatives, and establishing dedicated shortage committees to prevent ad-hoc, risky decision-making.
Will the $1.2 billion government investment fix the problem quickly?
Probably not. While the funding for domestic manufacturing is a positive step, experts believe it will take 3-5 years before these new facilities are operational and producing medications at scale.