How to Assess Risk When Only Expired Medications Are Available
- Colin Hurd
- 3 March 2026
- 8 Comments
When you’re stuck with only expired medications on hand, the question isn’t just whether they’ll work-it’s whether using them could hurt you. You might be in a remote area, dealing with a power outage, or caught in an emergency where pharmacies are closed. Maybe you found an old bottle in the back of a cabinet after losing your prescription. Whatever the situation, you need to make a call: use it or risk harm. This isn’t about guessing. It’s about understanding what really changes after the date on the label-and what doesn’t.
Expiration Dates Don’t Mean “Useless After This Day”
The date printed on your medicine bottle isn’t a magic expiration bell. It’s a manufacturer’s guarantee: until this date, we promise the drug is at full strength and safe. But that doesn’t mean it turns toxic the next day. The U.S. Food and Drug Administration (FDA) has tested over 100 drugs in its Shelf Life Extension Program, and found that 90% of medications remain safe and effective up to 15 years past their expiration date-if stored properly. That’s not a rumor. It’s real data from military stockpiles kept in climate-controlled conditions.
But here’s the catch: most of us don’t store meds like the U.S. military. We keep them in bathroom cabinets, where humidity from showers and heat from pipes speed up degradation. A 2024 study in the PMC journal showed that medications stored in humid environments degrade 37% faster than those kept in cool, dry places. So while the FDA’s data is solid, your bottle might be far less stable.
Not All Medications Are Created Equal
Some drugs are forgiving when they expire. Others? They’re dangerous. The difference isn’t just about how long they last-it’s about what happens when they break down.
- Never use expired: Insulin, thyroid meds (like levothyroxine), birth control pills, and anti-platelet drugs (like aspirin or clopidogrel). Insulin can lose potency and cause dangerous blood sugar swings. Thyroid meds need precise dosing-too little or too much can trigger heart problems or extreme fatigue. Birth control pills may fail, leading to unintended pregnancy. Anti-platelet drugs losing strength could mean clotting risk isn’t controlled.
- High risk: Liquid medications, eye drops, injectables, and antibiotics. Liquids can grow bacteria. Eye drops might become contaminated. Antibiotics that are weak won’t kill the infection-they’ll just train bacteria to resist future treatment. The CDC warns these are the most likely to cause harm after expiration.
- Lower risk: Solid tablets like ibuprofen (Advil, Motrin), acetaminophen (Tylenol), antihistamines (Benadryl, Zyrtec), and some antacids. These tend to hold up well if kept dry and cool. Tylenol may lose up to 20% potency after its shelf life, but it won’t turn toxic. You might not get full pain relief, but you won’t get poisoned.
Washington State’s 2023 health report found that 68% of emergency visits involving expired meds were tied to insulin or cardiac drugs. That’s not random. It’s because these drugs demand exact dosing. A 10% drop in potency? For a painkiller, maybe okay. For insulin? Could land you in the hospital.
Check the Physical Condition-Even If It’s “Just a Few Months Old”
Look at the pill. Smell it. Feel it. If it’s changed, don’t use it.
For tablets: Are they cracked, discolored, or powdery? Has the coating turned sticky? That’s a sign moisture got in. If it smells weird-like vinegar, mildew, or chemicals-it’s breaking down. Tablets stored in heat can melt slightly and re-harden into odd shapes. That’s not normal.
Liquids? If they’re cloudy, have particles floating in them, or smell off, toss them. The CDC says expired liquids can produce toxic byproducts. Even if it looks fine, don’t risk it. No home test can confirm safety.
Topical creams: If they’ve separated, changed texture, or smell rancid, they’re no longer safe. Skin absorbs these directly-contamination here can lead to infection.
Time Matters-But Not Like You Think
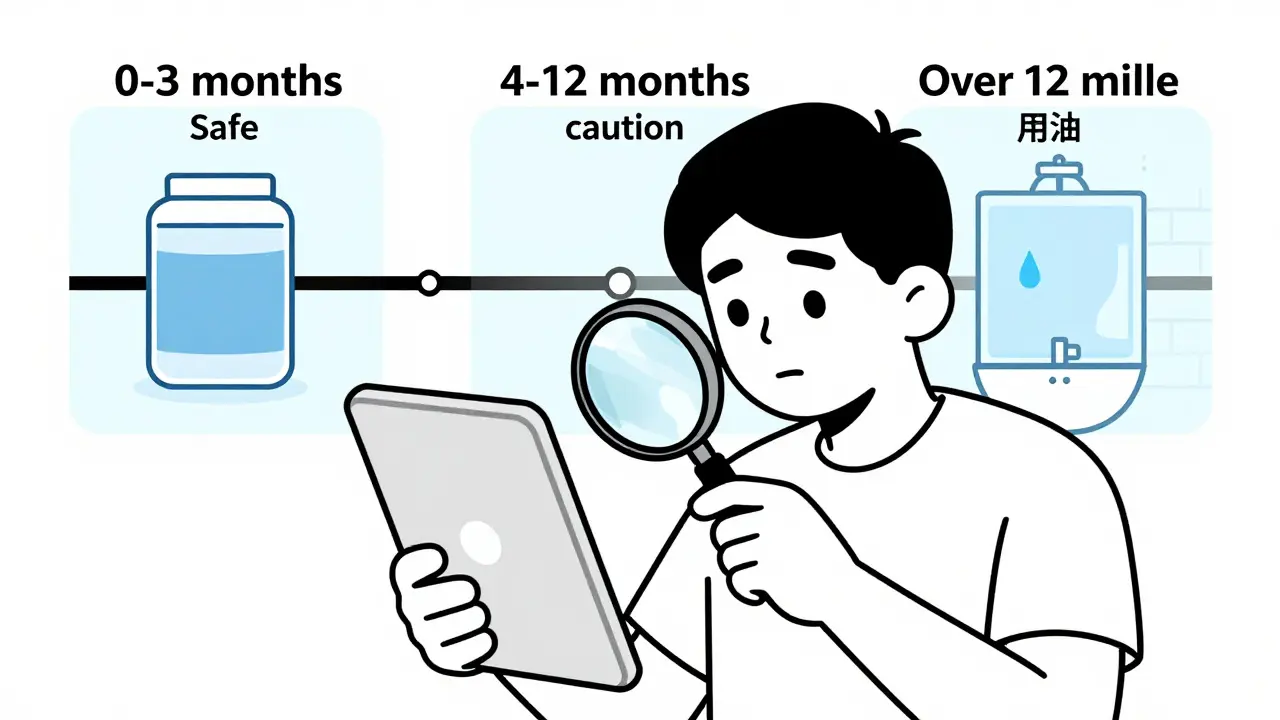
How long has it been expired? It’s not just “a year” or “two years.” It’s about how many months.
- 0-3 months past: For stable solids like ibuprofen or Tylenol, this is usually low risk. Potency loss is minimal. You might feel less relief, but it’s unlikely to cause harm.
- 4-12 months: Still okay for non-critical meds if they look fine. But avoid if you’re elderly, pregnant, immunocompromised, or treating a child.
- Over 12 months: The risk climbs sharply. Providence Health’s guidelines say this is the threshold where you should stop relying on expired meds-even for OTC painkillers. Storage conditions matter more now. If it was in a hot car or humid bathroom? Don’t use it.
Manufacturer data is more precise than general advice. Tylenol says its acetaminophen drops to 80% effectiveness after 2-3 years past shelf life. That’s not a guess. That’s lab-tested. If you know the brand, use their data. Don’t rely on “I heard it’s fine for 5 years.”
Storage History Is the Wild Card
You probably don’t know how your meds were stored before you got them. But you can guess.
Did it come from a pharmacy? Was it in a box, then moved to a windowsill? Was it left in a car during summer? Heat, light, and moisture are the three killers of medication stability. A 2023 Swedish Health Services review found that meds stored in bathrooms degrade 37% faster than those in a bedroom drawer. If your bottle was in the medicine cabinet above the sink? Assume it’s been exposed to steam and humidity every day for years.
Even if it’s only been expired for two months, if it was stored poorly? Treat it like it’s been expired for two years.
When Is It Okay to Use an Expired Med? Only in These Cases
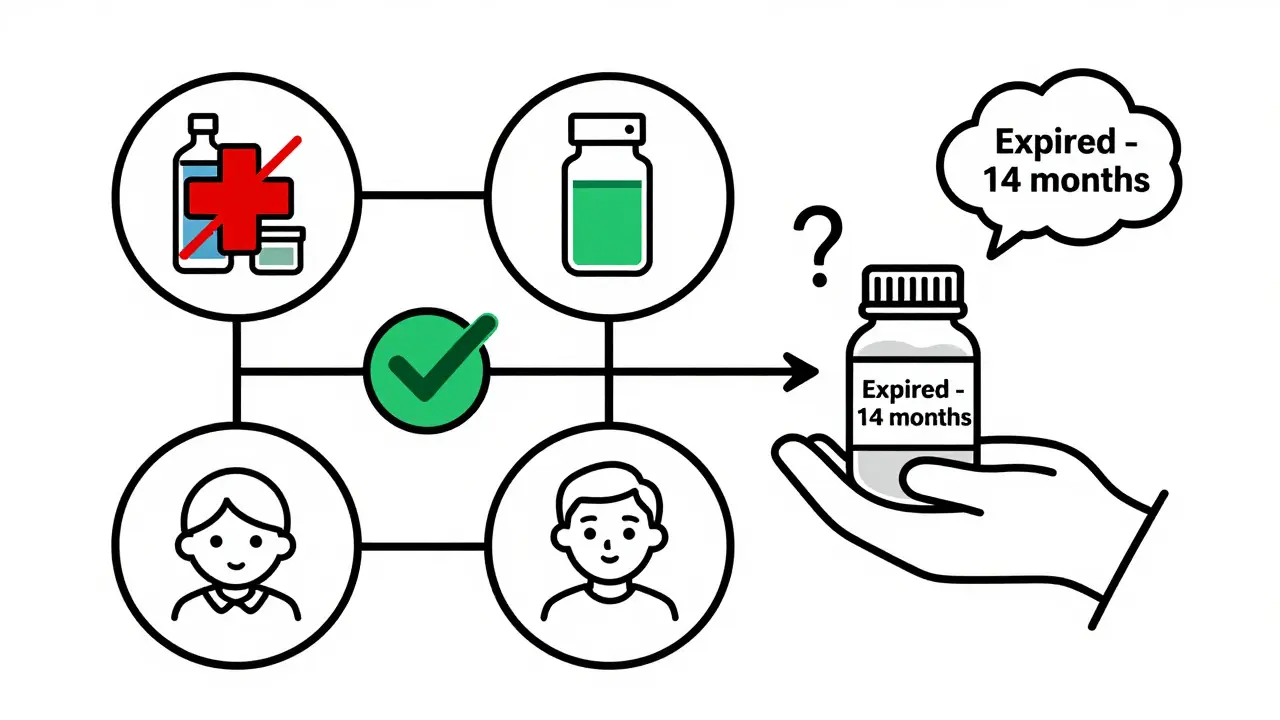
There’s no blanket rule. But there is a decision tree.
- Is it on the “never use” list? Insulin, thyroid meds, birth control, blood thinners? If yes-do not use. Period.
- Is it a liquid, eye drop, or injection? If yes-do not use. No exceptions.
- Is it a solid tablet or capsule? If yes, check its condition. No discoloration? No odor? No stickiness? Then proceed.
- How long has it been expired? Under 12 months? Maybe okay. Over 12 months? Skip it.
- What are you treating? Mild headache? Maybe. Severe infection? No. Fever in a child? No. Chronic condition? No.
- Who’s taking it? Elderly? Child? Pregnant? Immune system weak? Then skip it.
- Is there any alternative? Even if it’s a different brand, or a neighbor’s leftover OTC? Use that instead. Expired meds are the last resort.
Bottom line: If you’re using an expired drug because you have no other option, you’re taking a calculated risk. Not a smart one. But sometimes, you have no choice. In those cases, use the smallest effective dose. Watch for signs it’s not working. And get real medicine as soon as possible.
Why This Is a Systemic Problem
One in five emergency visits involving expired meds could have been avoided, according to Washington State’s 2023 data. That’s not just bad luck. It’s poor medication management.
Most people don’t rotate their medicine cabinet. They buy a new bottle, toss the old one into the drawer, and forget about it. A 2024 study found that the average household has at least 3 expired medications. Half of them are painkillers. The other half? Things people forgot they even had.
Fixing this isn’t about learning to use expired drugs. It’s about preventing the situation altogether. Check your cabinet every six months. Throw out anything expired. Don’t hoard “just in case.” Medicines aren’t canned food. They’re precision tools.
What’s Next? Maybe Better Tools
The FDA is funding research into portable devices that could test drug potency at home-using light spectroscopy to detect chemical changes. Think of it like a breathalyzer for pills. But as of October 2023, no such device was available to the public. Don’t wait for tech to save you. The tools you have now-your eyes, your sense of smell, your knowledge of storage-are your best defense.
Can expired medications make you sick?
Yes, but only in specific cases. Expired liquid medications, eye drops, or injectables can grow bacteria or break down into toxic chemicals. Antibiotics that have lost potency may not treat infection and can contribute to antibiotic resistance. For solid tablets like ibuprofen or Tylenol, you’re unlikely to get sick-just less relief. But if the pill looks strange, smells off, or has changed texture, it’s safer to avoid it entirely.
Is it safe to take expired Tylenol or Advil?
If they’re solid tablets, stored in a cool, dry place, and expired less than a year ago, they’re usually safe. Tylenol may lose up to 20% of its potency after expiration, but it doesn’t become toxic. Advil and Motrin follow similar patterns. But if the pills are discolored, crumbling, or have an odd smell, don’t use them. And never use expired liquid forms of these drugs.
Why do some drugs expire faster than others?
It depends on the formulation. Tablets are stable because they’re dry and sealed. Liquids, creams, and injectables contain water or solvents that can break down or grow bacteria. Insulin and thyroid meds are proteins or hormones that degrade quickly with temperature changes. Antibiotics are chemically unstable and lose effectiveness fast. Manufacturers test each drug type differently, which is why expiration dates vary.
Can I use expired medication in an emergency?
Only as a last resort. If you have no other option and are treating a minor issue like a headache or mild allergy, a recently expired solid tablet might be okay. But never use expired insulin, birth control, antibiotics, or heart medications in an emergency. The risk of failure is too high. If you’re unsure, wait-even if it’s inconvenient. Better to wait than to risk serious harm.
How can I prevent having expired meds on hand?
Check your medicine cabinet every six months. Throw out anything expired, discolored, or smelling odd. Don’t stockpile “just in case.” Buy only what you need. Store meds in a cool, dry place-not the bathroom. Keep them in their original containers with labels intact. And always ask your pharmacist when you pick up a new prescription: “When should I throw this out?”



Comments
Milad Jawabra
Let’s be real-most people keep meds in the bathroom like it’s a damn sauna. I’ve seen expired ibuprofen that looked like it survived a monsoon. But guess what? I used a 3-year-old Tylenol during a power outage last winter and lived to tell about it. No side effects, just a slightly slower pain drop. If it looks, smells, and feels normal? It’s probably fine. Don’t let fear-mongering scare you into suffering needlessly.
March 5, 2026 AT 04:22
Sharon Lammas
There’s something deeply human about holding onto medicine long after its label says it’s done. We cling to these little pills like talismans against chaos. The science says most are safe-but the real question isn’t chemical stability. It’s whether we’re clinging to control in a world that refuses to be controlled. Maybe the expiration date isn’t on the bottle. Maybe it’s on the belief that we can predict, prepare, and outsmart every disaster.
March 7, 2026 AT 02:14
Diane Croft
You’ve got this. Seriously. Knowledge is power, and you’re already ahead of most people just by asking the right questions. Keep checking your cabinet, stay calm, and trust your instincts. You’re not just surviving-you’re learning how to take care of yourself, even when things get messy. That’s strength.
March 7, 2026 AT 15:53
Tildi Fletes
Per FDA guidelines, the expiration date reflects the point at which the manufacturer can no longer guarantee potency under labeled storage conditions. However, degradation kinetics vary by molecular structure. For instance, acetaminophen undergoes hydrolytic decomposition primarily via ester cleavage, with a half-life of approximately 4.2 years under accelerated aging conditions (40°C/75% RH). In contrast, insulin, a polypeptide, denatures irreversibly above 30°C. Therefore, the risk profile is not temporal but physicochemical. Storage history is the primary variable, not calendar time.
March 8, 2026 AT 12:21
Siri Elena
Oh wow. A whole essay on whether your Advil is still ‘good.’ Let me grab my lab coat and pH meter before I take a Tylenol. Truly, the pinnacle of modern self-reliance: judging a pill by its color and sniffing it like a sommelier. Next up: ‘How to Assess the Moral Integrity of Your Antihistamine.’
March 10, 2026 AT 04:17
Divya Mallick
Listen. In India, we’ve been using expired medicines for decades because the system doesn’t care if you live or die. We don’t have luxury of ‘cool, dry places.’ We have a 45°C summer, a leaking roof, and a pharmacy that charges 300 rupees for a 10-pill pack. So yes, I’ve taken expired insulin. I’ve taken expired antibiotics. I’ve taken expired painkillers. And I’m still here. Your ‘guidelines’? They’re written by people who’ve never had to choose between medicine and rent. Don’t lecture us about safety when you’ve never lived without it.
March 11, 2026 AT 03:53
Pankaj Gupta
Divya raises a valid point about systemic inequity. However, it is imperative to distinguish between necessity and negligence. While cultural and economic contexts may compel individuals to use suboptimal pharmaceuticals, the biomedical risks remain quantifiable and non-negotiable. Antibiotic resistance, for instance, is not a political issue-it is a biological consequence of partial dosing. One may survive using expired insulin, but one also contributes to a broader public health crisis. Compassion must be paired with responsibility.
March 11, 2026 AT 14:37
Chris Beckman
my cousin took a 7 year old xanax and said it was like a warm blanket. idk if that’s a thing but i think we’re all just guessing at this point. also why do people store meds in the bathroom? it’s not a sauna. unless you’re taking a bath while you’re on fire. then maybe. lol
March 12, 2026 AT 00:08