Steroid Hyperglycemia in Diabetes: How to Adjust Insulin and Medications

- Colin Hurd
- 18 March 2026
- 8 Comments
Steroid Insulin Adjustment Calculator
Steroid Adjustment Calculator
Calculate insulin adjustments based on steroid dose and current regimen
Adjustment Results
Enter your current insulin dose and steroid dose to see adjustment recommendations
Important Safety Notes
1. Do NOT adjust insulin without consulting your healthcare provider
2. Always check blood glucose 4-6 times daily when on steroids
3. Pause SGLT2 inhibitors during steroid therapy
4. Reduce insulin slowly during steroid tapering (10-20% per 10mg steroid reduction)
Why Steroids Make Blood Sugar Spike in People with Diabetes
When you’re on steroids-whether it’s prednisone, hydrocortisone, or dexamethasone-your blood sugar doesn’t just go up a little. It can shoot through the roof. This isn’t a coincidence. It’s biology. Steroids, especially glucocorticoids, directly interfere with how your body uses insulin. They make your liver dump more glucose into your bloodstream, block insulin from doing its job in muscle and fat cells, and even reduce insulin production from your pancreas. For someone with diabetes, this is like adding fuel to a fire that’s already burning. A 2012 study in the Journal of Clinical Endocrinology & Metabolism found that over 50% of patients on high-dose steroids developed hyperglycemia. In some cases, that number jumped to 86%-meaning nearly everyone on high steroids will see their glucose climb.
And here’s the tricky part: it’s not just fasting glucose that goes up. Most of the spike happens after meals. That’s because steroids peak in your system 4 to 8 hours after you take them. If you’re taking one daily dose in the morning, your blood sugar will likely be highest after breakfast and lunch-not dinner. Relying only on morning fasting readings? You’ll miss nearly 20% of the problem.
How Much More Insulin Do You Really Need?
If you already have type 2 diabetes and you’re starting steroids, don’t be surprised if your insulin needs jump by 30% to 50%. For some, it’s even more. A 2021 review from Great Ormond Street Hospital showed pediatric patients on high-dose steroids needed 25% to 40% more total daily insulin, with the biggest increases in mealtime doses. Why? Because the sugar spikes happen after eating, not overnight. That means you need more rapid-acting insulin to cover meals, not just more long-acting insulin to keep baseline levels steady.
Here’s a real-world rule of thumb: for every 20 mg of prednisone (or its equivalent) you’re taking, expect to increase your total daily insulin by about 20%. For doses above 50 mg, that increase can hit 50% or more. A 2014 study tracking over 11,000 patients found that those on 100 mg of hydrocortisone daily were over five times more likely to need insulin than those not on steroids. And if you’re on 120 mg or more? Your risk jumps to over ten times higher.
But here’s the mistake most people make: they just add more insulin and never take it back off. That’s dangerous. When the steroid dose starts to come down, your insulin needs drop too-sometimes fast. A 2019 Johns Hopkins study found that 18% of patients readmitted to the hospital within 30 days of stopping steroids had low blood sugar. Why? Their insulin doses hadn’t been reduced. The same thing happens with oral meds. Metformin might help a little, but it won’t cut it alone. GLP-1 agonists? They can help, but not if your pancreas is already shut down by steroid damage. Insulin is still the go-to.
When to Use Basal-Bolus Over Sliding Scale
Sliding scale insulin-where you give a fixed dose based on your blood sugar reading-is outdated for steroid hyperglycemia. It’s reactive, not proactive. You’re waiting for a spike to happen before acting. By then, your glucose is already at 250 mg/dL or higher. That’s not control-that’s damage control.
The better way? Basal-bolus. That means a long-acting insulin (like glargine or degludec) for background needs, plus rapid-acting insulin (like lispro or aspart) before meals. This lets you match insulin to the steroid’s rhythm. If you take prednisone at 8 a.m., your glucose will peak around noon and again around 4 p.m. So you need more insulin at breakfast and lunch. Dinner? Often, you don’t need extra. This is why many endocrinologists recommend checking your glucose before breakfast, 2 hours after breakfast, before lunch, 2 hours after lunch, before dinner, and at bedtime. That’s six checks a day. Some patients on high-dose steroids do eight.
Continuous glucose monitors (CGMs) are game-changers here. A 2021 Dexcom case series showed users adjusted their insulin 37% more accurately than those using fingersticks. Why? Because CGMs show trends, not just snapshots. You can see that your glucose is climbing at 11 a.m., even if you haven’t eaten yet. That tells you the steroid is kicking in. You don’t have to wait for a high reading to act.
What About Other Medications? Metformin, SGLT2 Inhibitors, and More
Metformin? It helps with insulin resistance, so it’s still useful. But it won’t stop a steroid spike. If you’re on metformin and start steroids, you’ll likely still need insulin. Don’t stop metformin unless your doctor says so-it can help with weight and liver fat, especially if you’re on long-term steroids.
SGLT2 inhibitors (like empagliflozin or dapagliflozin)? Be careful. These drugs make your kidneys flush out sugar. Sounds good, right? But steroids make you dehydrated. Combine that with SGLT2 inhibitors, and you increase your risk of diabetic ketoacidosis (DKA)-even if your blood sugar isn’t super high. The FDA has warned about this. For short-term steroid use, pause SGLT2 inhibitors. Resume only after the steroid is fully tapered.
GLP-1 agonists (like semaglutide)? They’re great for weight and long-term control, but they’re slow to work. If you’re on a short steroid course (7-14 days), they won’t help much. If you’re on steroids for months, they can be part of the plan-but not the main one. Insulin is still the frontline.
And watch out for other drugs. Tacrolimus, used after transplants, makes steroid-induced hyperglycemia even worse. It blocks insulin release. Mycophenolate? Linked to insulin resistance in lupus patients. Even low magnesium can make things worse-each 0.1 mg/dL drop in magnesium raises your risk of high blood sugar by 10-15%. If you’re on long-term steroids, get your magnesium checked.
How to Adjust When Steroids Are Tapering
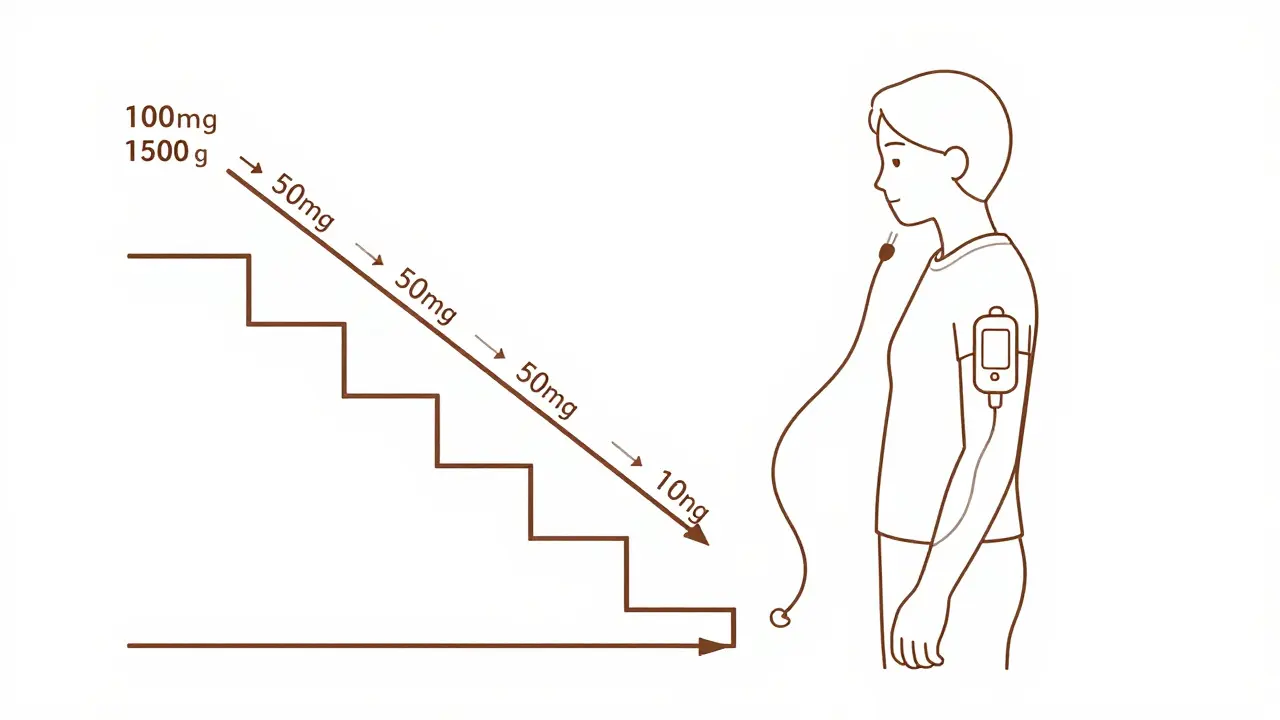
This is where most people fail. You’re feeling better. The steroid dose is dropping. You think you can go back to your old routine. But your body is still adjusting. Insulin needs don’t fall in a straight line. They drop unevenly. One day you’re on 10 mg of prednisone, the next you’re on 5 mg. Your insulin might need to drop 20% after each 10 mg reduction.
Here’s a simple guide: reduce your total daily insulin by 10-20% for every 10 mg you cut from your prednisone dose (or equivalent). If you were on 60 mg of prednisone and now you’re on 40 mg, cut insulin by 20%. If you’re down to 10 mg? You might need to cut insulin by 50% or more. Don’t guess. Check your glucose 4-6 times a day. If your levels are dropping too fast, slow the reduction.
And don’t forget: if you were on insulin for the first time because of steroids, you might not need it at all after tapering. Some people with steroid-induced diabetes go back to normal glucose control once the steroid is gone. But you need to monitor for at least 3 months. Your doctor should check your HbA1c and fasting glucose after you’re off steroids. If it’s normal, you might not have type 2 diabetes-you just had a temporary spike.
Tools and Technology Making a Difference
Hospitals are starting to use tools that automate this. The EndoTool system, now used in over 280 U.S. hospitals, adjusts insulin doses based on steroid type, dose, and current glucose levels. It’s reduced hyperglycemia by 27%. Apps like Glytec’s eGlucose system cut hypoglycemia events by 33% during steroid tapering by predicting insulin needs ahead of time.
And the future? Machine learning. A 2023 study in The Lancet Diabetes & Endocrinology used AI to predict insulin needs based on steroid dose, BMI, and HbA1c. It was 85% accurate. That’s not science fiction-it’s happening now. Pilot programs at Mayo Clinic are linking CGMs directly to EHRs, so when you take your steroid, your insulin pump gets a nudge: “Increase lunch dose by 30%.”
What You Should Do Right Now
If you’re starting steroids:
- Check your blood sugar 4-6 times a day, especially after meals.
- Use CGM if you have it-it’s the most accurate way to track trends.
- Switch to basal-bolus insulin if you’re not already on it.
- Don’t increase insulin without knowing your steroid dose. A 20 mg dose of prednisone needs different insulin than 50 mg.
- When tapering, reduce insulin slowly and check glucose daily.
- Pause SGLT2 inhibitors until steroids are fully off.
- Ask your doctor to check your magnesium if you’re on steroids longer than 2 weeks.
If you’re unsure, don’t guess. Call your endocrinologist. Steroid hyperglycemia isn’t just “high sugar.” It’s a unique, time-sensitive problem. Get it right, and you avoid hospital visits. Get it wrong, and you risk DKA, nerve damage, or hypoglycemia during tapering. This isn’t something to wing.


Comments
lawanna major
This is one of those posts that makes you feel seen. I’ve been on prednisone for lupus flares, and the blood sugar spikes were terrifying. I didn’t realize the peak was after lunch until I started using my CGM. Now I adjust my insulin before I even eat-because the steroid is already working. It’s not about reacting. It’s about anticipating. And honestly? This level of detail in medical advice is rare. Thank you for writing this like a human who’s been through it.
Also, magnesium. I didn’t know that. Got tested last week. My levels were low. Supplemented. My fasting sugars dropped 18 points. Small things matter.
March 18, 2026 AT 21:42
Linda Olsson
Of course the pharmaceutical industry loves this. Steroids are cheap. Insulin? Expensive. Basal-bolus? Requires monitoring. CGMs? Even more expensive. And suddenly, every diabetic on prednisone becomes a lifelong insulin user. Convenient, isn’t it? They don’t tell you about the natural ways to counteract steroid-induced insulin resistance-like intermittent fasting, magnesium, and chromium. No, they push the pump. Profit over physiology.
March 20, 2026 AT 03:36
Ayan Khan
As someone from India where steroid use is widespread due to cost and accessibility, I’ve seen this play out in clinics where patients are given prednisone without any glucose monitoring. The result? Diabetic ketoacidosis in patients who never had diabetes before. This article is vital. But it must be translated into regional languages. The real challenge isn’t the science-it’s the delivery. We need community health workers to explain this in simple terms. Not just doctors in white coats. People in villages need to know: if you take steroids, check your sugar. Even if you feel fine.
March 20, 2026 AT 22:34
Emily Hager
I find it profoundly disturbing that the medical establishment continues to treat steroid-induced hyperglycemia as a mere ‘adjustment’ rather than a systemic failure of preventive care. The fact that we are now recommending insulin titration based on a drug’s pharmacokinetics rather than addressing the root metabolic disruption is a testament to our reliance on pharmaceutical band-aids. One must ask: why are we not researching steroid alternatives with lower glycemic impact? Why are we not studying the long-term beta-cell damage caused by repeated steroid exposure? This is not medicine. This is damage mitigation.
March 22, 2026 AT 00:51
Melissa Starks
Okay I just wanna say I’m so glad I found this. I’m a type 2 diabetic and I got a 10-day prednisone pack last month. I thought I was fine because my fasting sugar was okay. Then I started feeling wiped out after lunch. My CGM showed I was hitting 280 after every meal. I was like… why am I so tired?? I didn’t even know I needed more insulin at lunchtime. I just added 2 units to my lunch dose and boom. My energy came back. I’m still scared to taper though. I’m scared I’ll crash. I’ve been checking 6 times a day. I don’t even go out anymore. I just stare at my glucose graph like it’s my baby. Also I got my magnesium checked and it was low. Took a supplement. My numbers improved. I’m so glad someone said that. I thought I was the only one who noticed.
March 22, 2026 AT 23:06
Lauren Volpi
Ugh. Another ‘trust the science’ lecture. Real talk: most of these patients are on steroids because they can’t afford the real treatment. The real problem isn’t insulin dosing-it’s that the healthcare system forces people into this mess. And now we’re telling them to buy CGMs and insulin pumps? Meanwhile, the same people are choosing between rent and metformin. This isn’t medicine. It’s a luxury guide for the insured.
March 24, 2026 AT 04:32
Melissa Stansbury
I just want to say thank you for mentioning the 18% readmission rate from hypoglycemia during tapering. My mom got discharged after a 3-week steroid course and they told her to go back to her old insulin dose. She went into a coma two days later. We almost lost her. No one told her the insulin had to come down. No one. Not even her endo. This isn’t just advice. It’s a life-or-death protocol. Please, if you’re reading this: if you’re tapering, check your glucose before bed. If it’s below 90, eat something. Don’t wait. Don’t assume. Don’t trust the ‘normal’ numbers. You’re not normal anymore.
March 24, 2026 AT 19:01
Alexander Pitt
The EndoTool and eGlucose systems are real. I work in an ICU that uses them. We saw a 40% reduction in hyperglycemic events and 50% fewer hypoglycemic episodes in steroid patients. The AI models are trained on real-time data-steroid dose, weight, HbA1c, meal timing, even sleep patterns. It’s not magic. It’s math. And yes, it’s working. I’ve seen patients who were on 100 units of insulin daily drop to 30 within 10 days of tapering, with zero lows. The tech isn’t perfect, but it’s the closest we’ve gotten to personalized, dynamic insulin therapy. Stop thinking of this as ‘insulin adjustment.’ Think of it as metabolic recalibration. And if you’re not using a CGM? You’re flying blind.
March 25, 2026 AT 08:37